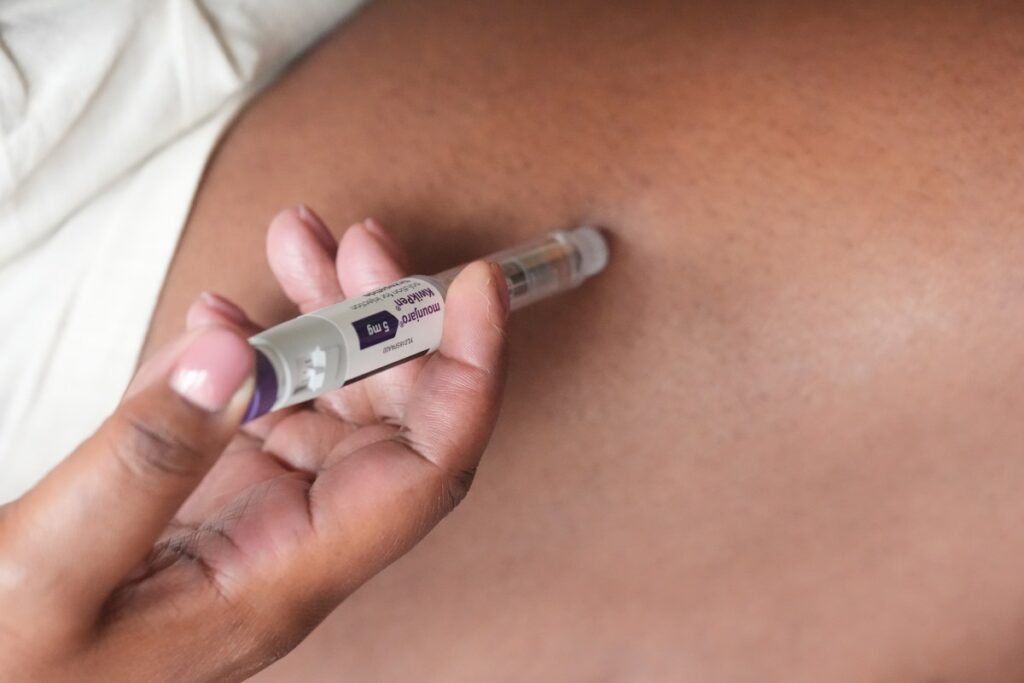
As GLP‑1 weight‑loss drugs move into the medical mainstream, experts say they may pose under‑recognized risks for some patients with complex chronic conditions—underscoring the need for careful screening and close medical supervision.
GLP-1s like Ozempic and Wegovy have become increasingly popular, with one in eight Americans using them as of March 2026, according to data from Statista. Their rise has coincided with a decline in U.S. obesity rates, though experts caution multiple factors are at play.
The medications are approved for the treatment of type 2 diabetes and obesity and are widely considered effective when prescribed appropriately. However, clinicians say their effects may not be uniform across all patient populations.
How Do GLP-1s Work?
GLP‑1, also known as glucagon‑like peptide‑1, is a hormone produced naturally by the body. After eating, it helps regulate blood sugar by stimulating insulin release, suppressing glucagon, slowing gastric emptying and increasing feelings of fullness.
Lily Spechler, a dietitian specializing in long COVID and other chronic conditions based in New Jersey, told Newsweek that GLP-1 drugs therefore work by “mimicking the hormone.”
For many, these drugs have huge benefits. However, “it’s not a one-size-fits-all approach,” Spechler said, as for some these drugs may not be suitable.
Increased Risk Of Gastroparesis
As GLP‑1s slow gastric emptying, they can increase the risk of gastroparesis—a condition in which the stomach empties too slowly, causing symptoms such as nausea, vomiting, bloating and abdominal pain—particularly in patients already prone to digestive motility issues.
Certain patients, like those with the chronic connective tissue condition Ehlers-Danlos Syndrome (EDS), may already be susceptible to having gastroparesis.
Those with the condition have connective tissue, something which lines most of the body, that works differently to someone without the condition, and means they are more likely to experience digestive issues that result in food moving irregularly through the gut.
Patients with Postural Orthostatic Tachycardia Syndrome (PoTS), an autonomic nervous system disorder, may also experience similar issues.
Digestion relies on the parasympathetic “rest and digest” state, and in PoTS, altered autonomic regulation may disrupt this process, contributing to gastrointestinal symptoms in some patients, Spechler explained.
Spechler said that for patients experiencing gastroparesis while still benefiting from GLP‑1s, dietary adjustments may sometimes be considered under clinical guidance, such as a low‑residue, small‑particle diet designed to help food move more easily through the gastrointestinal tract.
Issues With Curbing Appetite
Curbing appetite by tricking the brain into thinking you’re full more of the time can come with risks, particularly for those with chronic conditions like long COVID, PoTS and EDS.
Typically people with these conditions “are going to especially need more protein to help maintain connective tissue integrity,” Spechler said. They also “need enough calories to tamper down the chronic inflammatory state” they are experiencing, she added.
While there is no clear consensus on calorie needs for long COVID patients, Spechler said that she often advises her patients to eat around 10 to 15 percent more calories than their TDEE (Total Daily Energy Expenditure) calculated baseline due to the increased metabolic demands of their body in light of symptoms like temperature dysregulation, tachycardia and breathlessness.
So while these drugs can have a positive impact on inflammation by stabilizing blood sugar, Spechler said, there’s a “big question mark” around whether they could also have a negative effect on inflammation if metabolic needs are not met.
Impacts Of Sudden, Drastic Weight Loss
Sudden weight loss for some patients may also be problematic, especially if it exceeds the more than the one to two pounds per week health advisory bodies commonly advise. “If you go far above that, you’re at higher risk of losing some of your lean muscle mass and some healthy body tissue in addition to fat loss,” Spechler said.
She said rapid weight loss can disrupt electrolyte balance — particularly important for patients with conditions like PoTS — and some peer‑reviewed studies suggest it may temporarily increase circulating levels of persistent organic pollutants (POPs), chemicals stored in fat tissue, though the clinical significance of this remains under investigation.
For those with hypermobile EDS, or hEDS, losing muscle mass can also be a huge problem as patients with the condition rely on stronger muscles as “a critical component in managing joint stability and symptoms,” Lisa Becker-Schmall, a physical therapist with specialism in PoTS and hEDS, told Newsweek.
“As many patients with hEDS are also women, maintaining muscle mass for overall health and longevity is even more critical,” she added.
What The Experts Advise
While there are some concerns about using weight loss injectable medications for certain patients, that’s not to say they don’t have their place in the healthcare space.
“I think GLP-1s are a useful medication for some people, some of the time, and I am excited to see data that helps us clarify the best candidates,” Becker-Schmall told Newsweek. She said like any new medication or treatment, “there are a number of unknowns” that remain and need to be clarified through further research and investigation.
She added that for anyone determined to be a good candidate for a GLP-1, particularly those with hEDS, “a strong care team is a non-negotiable,” so that the patient has professionals reviewing their nutrition, bone density and muscle mass, and someone managing dosing and symptoms.
“The most successful clients I’ve seen on a GLP-1 with hEDS have had all three working together: dietician, rehab coach, and referring doctor,” she said.
Taylor Goldberg, a hypermobility coach based in Colorado, also told Newsweek that from what she’d seen with her patients, “working with a registered dietician seems to be the number one thing that can benefit patients,” in order to provide them with support to mitigate risks around malnutrition and potential adverse reactions to the drugs.
Goldberg added that it is also “too early” to have more than “opinions” about these drugs, as more data is needed to understand the whole-body impact of GLP-1s.
It is also important to know that people with EDS – and many other chronic conditions – will have “differing side effects, symptoms, allergies, and tolerances,” so how patients with the condition will tolerate different medications, like GLP-1s, cannot be generalized, Dr. Bernadette Riley, director of the Ehlers-Danlos Syndrome/Hypermobility Treatment Center at the New York Institute of Technology College of Osteopathic Medicine, told Newsweek.
For patients who decide not to use GLP‑1s following medical evaluation, Spechler said there are other approaches that may support weight management, including diet and lifestyle changes.
As GLP‑1 use continues to grow in the U.S., experts say the key question is not whether the drugs work, but who they are best suited for — reinforcing the importance of individualized treatment decisions and close medical supervision.
In a polarized era, the center is dismissed as bland. At Newsweek, ours is different: The Courageous Center—it’s not “both sides,” it’s sharp, challenging and alive with ideas. We follow facts, not factions. If that sounds like the kind of journalism you want to see thrive, we need you.
When you become a Newsweek Member, you support a mission to keep the center strong and vibrant. Members enjoy: Ad-free browsing, exclusive content and editor conversations. Help keep the center courageous. Join today.
Read the full article here